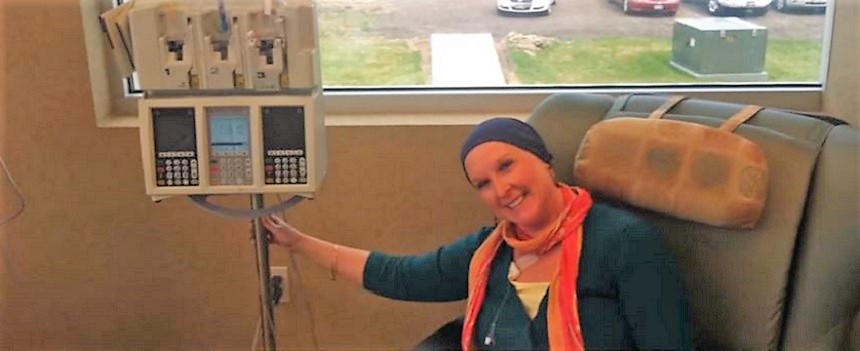
Diane: Psychological care for cancer patients
The views and opinions expressed in following story are those of the author and do not necessarily reflect the opinions of Mental Health Colorado.
When I asked my medical oncologist if she could refer me to a counselor who understood what it was like for me, a middle aged, high-strung female business executive who needed to be in control, to experience breast cancer, she couldn’t help me.
 Cancer. An ugly, frightening word. Of all the words in my vocabulary, it’s the word I hate most. Typically, when I say the word, I precede it with an adjective that’s not appropriate to print.
Cancer. An ugly, frightening word. Of all the words in my vocabulary, it’s the word I hate most. Typically, when I say the word, I precede it with an adjective that’s not appropriate to print.
I had a run-in with intermediate stage breast cancer in 2015, and I am a different person now. A woman with six fewer axilla lymph nodes, a thicker head of hair and chronic lymphedema in my left hand, but I am alive and grateful. My cancer experience was, by far, the most traumatic event of my life to this point.
During my 10 months of treatment, which started off with 16 chemotherapy infusions, my emotions swerved in every imaginable direction. My support network was strong, I had a supportive husband and I had every reason to believe that I would survive the treatment and my cancer would go into remission. Which, thankfully, it did. But, I sank into a sad, bored state near the end of chemo and remained parked there until the end of treatment.
When I asked my medical oncologist if she could refer me to a counselor who understood what it was like for me, a middle aged, high-strung female business executive who needed to be in control, to experience breast cancer, she couldn’t help me. She said that many licensed practitioners in the psychology field typically don’t receive specialized oncology training while pursuing their degrees – they must seek it out on their own, usually at the post-doctoral level. In addition, if I could find a counselor who understood cancer, my health insurance likely would not cover their service, assuming they even accepted insurance.
Despite my grumpy, bald state and my depleted energy levels, I set out to discover why so little attention was being paid to the psychological and emotional sides of cancer. What I was discovered is that health psychology, in general, is becoming more prevalent in human-centered healthcare, but we have a long road ahead.
The National Institute of Health projects that one in two men, and one in three women, will get some form of cancer in their lifetime. This staggering statistic is what prompted me to be a catalyst for positive change. In early 2016, I founded a specialty at the Graduate School of Professional Psychology at the University of Denver. The specialty, called the Center for Oncology Psychology Excellence, or COPE, is the first graduate-level specialty of its kind in the country.
Anxiety, depression and stress have many triggers, and cancer is just one of those triggers. But, thanks to the work of Mental Health Colorado, we are bringing attention to the benefits of addressing the psychological challenges of medical conditions.
— Diane Simard
———————————————————–
DONATE TO MENTAL HEALTH COLORADO
More than 500,000 Coloradans lack the mental health care they need. You can change that. For more than 60 years, Mental Health Colorado has led the charge in promoting mental health, ending stigma, and ensuring equitable access to mental health and substance use services. It’s life-changing work. Your contribution makes it possible.